Osteoporosis is a very common disease caused by loss of bone. The bones become thin and are thus much more liable to fracture.
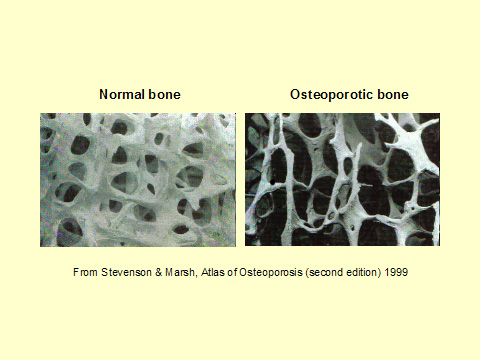
Osteoporosis is a very common disease caused by loss of bone. The bones become thin and are thus much more liable to fracture.

Causes
The maximum amount of bone in the skeleton (peak bone mass) is achieved soon after linear growth ceases, usually in the late teens. Peak bone mass is largely determined by genetic (inherited) factors, and thus a family history of osteoporosis may signify increased risk for developing the disease. The skeleton is kept healthy throughout life by processes which remove old bone tissue and replace it with new bone tissue (bone remodelling). The two processes of bone breakdown and bone formation usually balance each other so that bone mass is neither lost nor gained. Bone loss, which may result in osteoporosis, occurs when the process of bone breakdown exceeds that of bone formation. Bone loss occurs in all women following the menopause, and postmenopausal osteoporosis eventually affects 1 in 3 women. In men, bone loss occurs gradually with aging. Other causes of osteoporosis include overactive thyroid or parathyroid glands, certain cancers and leukaemias, rheumatoid arthritis, and treatments such as corticosteroids. Osteoporosis is less common in men, but can be due to lack of testosterone.
Effects
Bone loss itself does not cause any symptoms, and people losing bone for any reason are not aware of it. Fractures most commonly occur in the spine, wrist and hip, but can also occur in the ribs, pelvis, shoulder and ankle. Fracture causes immediate and often quite severe pain at the site. This pain can persist for several weeks but eventually resolves. More persistent pain, usually in the back, is usually due to bony deformity which produces a local arthritis, or sometimes due to microscopic fractures continually occurring. Osteoporotic fractures usually heal quite normally. Hip fracture is the most important osteoporotic fracture because it requires hospitalisation and usually a surgical operation, and it carries an increased early death rate.
Diagnosis
Osteoporosis may be suspected in someone who sustains a fracture after fairly minimal trauma. An X-ray may reveal the presence of spinal fractures but osteoporosis is often difficult to detect on plain X-rays in those who have not yet fractured. The best diagnostic procedure is to have a measurement of bone mineral density. This is performed on a dual-energy X-ray absorptiometry (DEXA) machine. It is a non-invasive procedure which takes just a few minutes to perform, and gives an almost negligible radiation exposure. Other procedures, such as using ultrasound (sound-wave) assessments, are less reliable.
Treatment